– as second round of MDA begins today
It is 8 o’clock Tuesday morning at the Vector Control Services Unit of the Georgetown Public Hospital Corporation (GPHC), and that means it is time for ‘Filaria Clinic’.
That morning, Bibi [not real name] struggled to bring her elderly brother, Ram [not real name] inside of the clinic because the wheelchair he was in makes it difficult to get him up the two short steps and through the narrow doorway. The lower half of his leg is swollen almost twice its regular size and he is unable to walk normally.
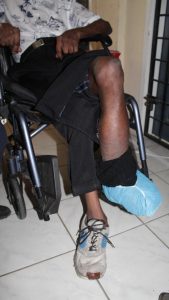
This enlargement of the tissues in Ram’s leg is the external manifestation of the chronic effects of Lymphatic Filariasis (LF), commonly known as Filaria. This is a disease that affects the body’s lymphatic system, which functions to remove unwanted fluids from the body and transports ‘lymph’– a fluid which contains white bloods cells that helps to fight infections.
“I’ve had it [Filaria] for five years,” Ram told the Guyana Chronicle.
THE DISEASE
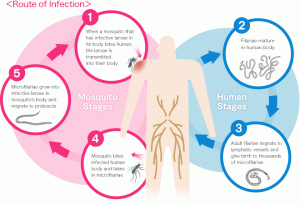
According to the World Health Organisation (WHO), LF is caused by infection through parasitic worms called nematodes, which are classified as ‘filarial worms.’ There are three main types of these worms:
- Wuchereria bancrofti- which causes Filaria in Guyana
- Brugia malayi
- Brugia timori
For countries in the Americas such as Guyana, the disease is transmitted by the culex mosquito.
Jenny [not real name], like Ram and the numerous others affected with Filaria, was bitten by the mosquito carrying the worms. Though she was diagnosed in 1992, after her tissues began swelling, the worms could have entered her body many years before.
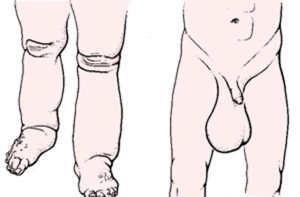
National Coordinator for the Elimination of Lymphatic Filariasis Campaign, Dr. Fabu Moses, explained that the conditions of LF may be asymptomatic, acute or chronic. According to her, there are no external manifestations for the asymptomatic conditions, though the body’s lymphatic system may still be affected. It may take several years however before this develops into a chronic condition, which includes the external manifestations of: lymphoedema (tissue swelling), elephantiasis (skin/tissue thickening) of the limbs and hydrocele (scrotal swelling).
Jenny made her way into the clinic with Ram on Tuesday morning, as well. Just about 26 years ago, in 1992, she discovered that her left leg began swelling, and that swelling was accompanied by high fever. The signs were worrying and she decided to visit the doctor. She was then diagnosed with Filaria.
Recounting the experience as though it was a mere month ago, Jenny explained that there were alot of mosquitos in her immediate surroundings and she wasn’t too fond of sleeping with mosquito nets. That proved to be detrimental to her health eventually.
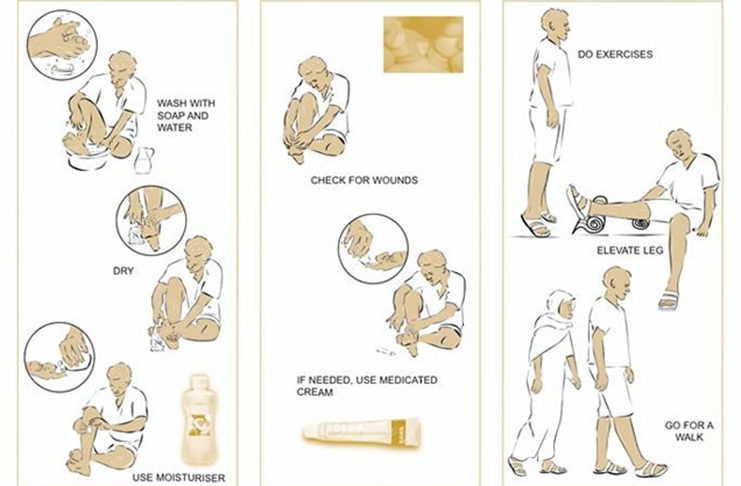
Over the years, she has became accustomed to the nets and the mosquito repellent. And more than that, she has adopted a ‘CARE’ regime to manage herself. Though there is no cure for Lymphatic Filariasis, CARE is an acronym used to guide its treatment.
C– cleaning the affected area
A– applying treatment
R– raising the affected area when sitting and above the level of the head when lying down
E– exercise
MDA: Round Two
Like Jenny and Ram, everyone exposed to mosquitos is susceptible to Filaria once they do not take measures to safeguard themselves. Filaria is also a neglected tropical disease which can be effectively controlled through public health approaches.
In 2017, the Ministry of Public Health (MoPH) in collaboration with the Ministry of Education and the Pan-American Health Organisation/ World Health Organisation (PAHO/WHO), launched a revitalised and re-conceptualised Mass Drug Administration (MDA) campaign to eliminate LF.
It is crafted under the title of “Let’s Prevent Filaria,” which stresses that the disease is NOT treatable, but citizens can safeguard against it through prevention.

The country had failed in a previous mandatory WHO programme to achieve the 65 percent coverage needed but through this new campaign, recorded a whopping 86 percent coverage in the four regions targeted, for the first round of the MDA.

“I was very encouraged by it [the 86 percent coverage],” Dr. Moses said and added: “I really think that people are starting to understand what it is what we’re doing and why it is we are trying to do this and I think that really contributed to the support we received.”
The National Coordinator also shared that the overall percentage of persons refusing to take the tablets ranged from three percent to eight percent.
The Dorothy Bailey Health Centre, located on South Road, Georgetown, was one of the many pill distribution centres across Guyana. In fact, this health centre was responsible for the largest catchment area in Georgetown and disseminated pills to 36,050 men, women and children- way more than what was anticipated.

Nurse Odette Adams- Thornton, who has oversight of the programme, underscored the importance of getting the buy-in from the public.
“I believe it’s how you sell the information and once you can give people accurate information about what you’re doing, they’ll be more receptive.
We have to train them [the pill distributors] to be able to deal with questions and reservations people have,” the nurse said while adding that this strategy contributed to the success of the centre’s MDA activities.
Crucial to the success of the MDA too, was the involvement of the Ministry of Education and schools, the nurse opined. During the previous MDA, the younger demographic has failed to meet the 65 per cent mark and this time around strategies were employed to assure this did not reoccur.
Dissent forms were given to children in schools so that their parents would indicate if they did not want their children to take the pills, but the nurse shared that many persons were confused and thought of it as an acceptance form instead. This was corroborated by Dr. Moses, who explained that because there was cognisance of this confusion, the form was renamed a “refusal form”.
Both Dr. Moses and Nurse Adams shared that they are confident that the campaign will be successful again, given the numerous public awareness strategies employed by the MoPH in conjunction with PAHO/WHO.
“We’ve seen an increase even from last year of persons calling to find out more- when they can get the tablets and how they can get it,” the doctor said.
And all in all, for the MDA to be successful once more, Dr. Fabu explained: “Once you have a large percent of the population, or as we say 65 percent of the population, being covered by these pills, even if there were to be an infected mosquito going around at that, infection rates would be much less. So that’s why we advocate for everyone to take it at the same time.”
The second of five rounds of the MDA begins on October 1 and will continue until early November.
WAY FORWARD
While the MDA was only conducted in Regions Three, Four, Five and 10- the regions identified as having the highest prevalence of Filaria from the previous campaign, this year the work will move to the other regions as well, Dr. Moses said.
“We still have the other regions with varying prevalence of Filaria,” Dr. Moses explained, adding “So what we’re going to be doing starting the same week in October is that we’re going to be going into regions One, Two, Six, Seven and Nine.”
This age group is being targeted because according to Dr. Moses, “Once we have realised that a child between that age has microfilariae antigen prevalence then we would be able to definitively say within the last 6-14 years there has been transmission in this area.”
And unlike the 2001 survey, the regions will be split up into smaller units or areas to identify smaller, at-risk populations because the regions are vast and a situation found in one area may not be representative of the entire region.
She explained that the blood test will only be administered if parents indicate their approval by signing the consent forms given and the test results will be provided immediately.
“If a child is found positive the parents are notified right away and they are directed to the health centre to get their care and treatment,” Fabu related and shared that if more than two per cent of the children surveyed in any area are infected with microfilariae, the MDA will be conducted in that area as well.

SAFEGUARD AGAINST FILARIA
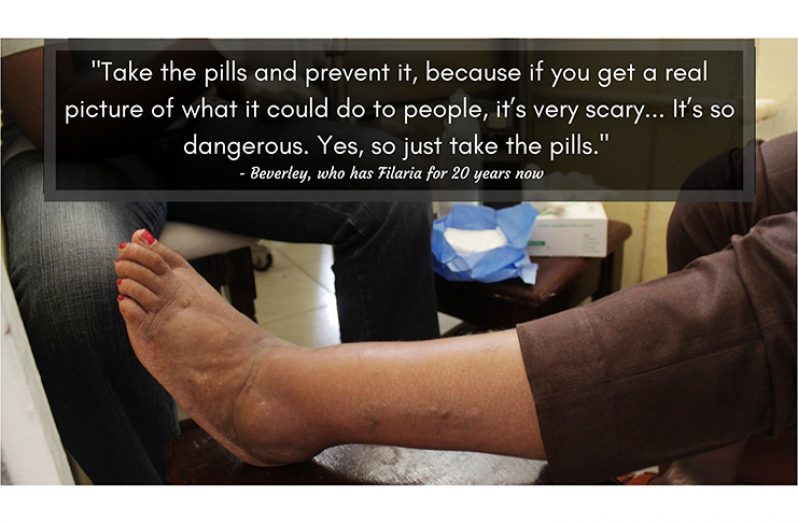
Back at the Filaria clinic, Beverley [not real name] just finished receiving the CARE treatment from Nurse Cheryl. She shared briefly her story of living with Filaria: “I got Filaria for 20 years. Sometimes I used to get an attack- swelling, fever and a little pain and it would take months to go down.”
But perhaps more importantly, Beverley heard that the MDA was moving into its second round and wanted to share her message to the general public.
“Take the pills and prevent it,” she encouraged and noted, “Because if you get a real picture of what it could do to people, it’s very scary. You see some patients who have it much worse [than her]; you wouldn’t believe that is the effect of Filaria. It’s so dangerous. Yes, so just take the pills.”
At the Dorothy Bailey Health Centre, the Nurse-in-charge (acting), Jean Bond stressed that participating in the MDA is not the only way of safeguarding against Lymphatic Filariasis.
“The understanding that we want people to have, is that prevention lies in their very surroundings: their yards, the waterways [and] the clogged drains. Sanitation along with repellents and mosquito nets are important,” Bond said.
Ram, Jenny and Beverley along with so many others are trying their best to live normal lives despite having the disease. With no cure, prevention is the best option and thus, safeguarding against this disease is essential.
Note: Names and faces of persons diagnosed with Lymphatic Filariasis were excluded upon request.



.jpg)