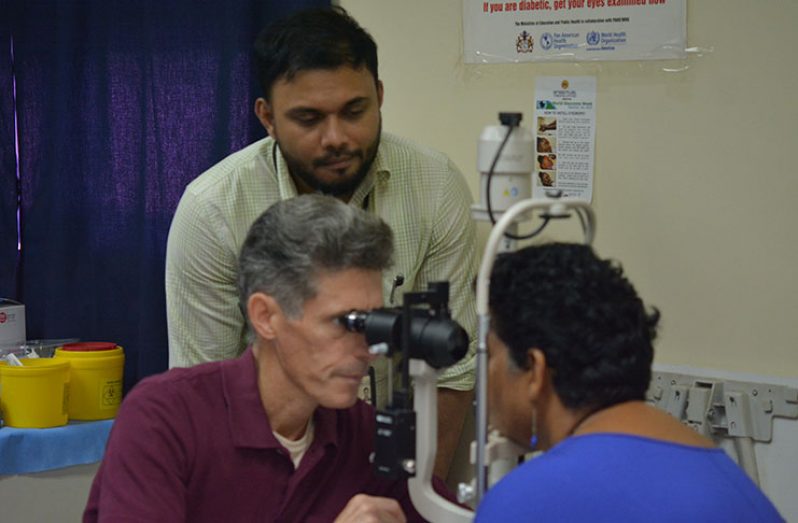
The intricate technique of Corneal Transplants
FOR many years, 67-year-old Jasoda Rajkumar had known that there was something drastically wrong with her right eye. It took her several years before she was diagnosed with Cataract – an eye disease that causes the lens of the eye to become cloudy preventing clear vision.

However, it was only in March 2017 that she underwent a surgery at the St. Joseph Mercy Hospital to remove the Cataract with high hopes of being able to see clearly again, but the situation worsened when the cornea in her right eye was damaged during the surgical procedure. The cornea is the transparent, dome-shaped surface of the eye that helps it to focus.
“It wasn’t so bad, but when I did the surgery, I couldn’t see at all in meh right eye,” the Enterprise, East Coast Demerara (ECD) woman said as she sat on a bench outside of the Eye Clinic at the Georgetown Public Hospital (GPHC).
Rajkumar’s case, however, is not unique to the Health Sector, according to US-based Corneal Transplant Specialist, Dr. Joseph Pasternak.
In an interview with the Pepperpot Magazine during his recent visit to Guyana, Pasternak said that cataract surgery is one of the many reasons that cause the cornea to fail. The World Health Organisation (WHO), on its website notes that: “Corneal visual impairment encompasses a wide variety of infectious and inflammatory eye diseases that cause scarring of the cornea, the clear membrane that covers the outside of the eye.”. It is said to be the fourth cause of blindness globally after cataract, glaucoma and Age-Related Macular Degeneration (AMD).

Zooming in on Rajkumar’s case, Dr. Pasternak said that late detection and subsequent removal of cataract very often result in damages to the cornea. “Some patients are not getting their cataract surgeries early enough. The cataract gets denser, harder and harder, making it more difficult to remove. The more difficult for it to be removed, the more complications there are,” he explained. “So the cloudy cornea is a complication of the cataract operation that shouldn’t cause the cornea to get cloudy but often does because in moving the cataract, it causes damages to the cornea.” In his estimation, approximately 20 percent of the people who undergo surgeries for cataract, experience Corneal Visual Impairment.
Other causes
Early detection of cataract and early surgeries would reduce the number of persons with Corneal Visual Impairment, Dr. Pasternak said. But this surgical procedure is not the only reason that causes the cornea to become cloudy.
Injuries, allergies, Keratitis, Keratoconus are among the conditions that also affect the

cornea, he pointed out. It was trauma that caused 26-year-old Elitizen Grant to rupture his cornea.
“He got a kick in his eye. He was playing with his nephew and he got kick straight in his eyes and he didn’t take it for nothing because the eye was alright,” Grant’s mother, Simone, recalled. The incident happened more than one year ago but it was only in June 2017 that the poultry farmer realised that his right eye was infected. “I had the red eye and from that I got this infection. It started running a set of cold,” Grant posited. After seeking medical attention at the GPHC Eye Clinic, the Williamsburg Corentyne farmer was informed by the doctors there that his cornea was torn. “They stitch it up for me but then I rubbed it and it loose out.”
The blurriness in his right eye had gotten worse.
Grant’s case, Dr. Pasternak said, was alarming. Contents of the eye including the pupil and iris were bulging out of the sac where the cornea had melted, the Cornea Transplant Specialist explained. “I was not expecting it,” he said.
While Rajkumar and Grant’s injuries were ‘man made’, 12-year-old Babita Kanhai and 26-year-old Shelana Britton were both diagnosed with Keratoconus – the thinning of the cornea.
The National Eye Institute (NEI) explains that “Keratoconus causes the middle of the cornea to thin, bulge outward, and form a rounded cone shape. This abnormal curvature of the cornea can cause double or blurred vision, nearsightedness, astigmatism and increased sensitivity to light,” NEI states. Kanhai and Britton, who hail from the Essequibo Coast and Bartica, respectively, were experiencing blurred vision.
Bringing relief
At the end of July, 2017, the Subraj Foundation, which is based in the US, teamed up with the GPHC’s Ophthalmology Department to conduct 16 corneal transplants either to restore vision, reduce pain or to save the eye.
Rajkumar, Grant, Kanhai and Britton were among the batch of patients from the GPHC Eye Clinic who benefitted from the surgical procedures.
According to the WHO, public health prevention programmes are the most cost-effective means of reducing the global burden of corneal blindness, however, once the cornea has been damaged, surgery by grafting of the cornea (corneal transplant) is currently the only curative treatment. A corneal transplant is a surgical procedure designed to replace part of the cornea with corneal tissue from a donor. It was, however, noted by WHO that access to this surgery has proven to be very difficult, even in developed countries, due to the lack of donors.
Here in Guyana, the corneal transplants were made possible by the Subraj Foundation with collaboration from GPHC and Eye Banks at no cost to the patients.
Dr. Pasternak, who had formed part of the US based team led by Dr. Rahul Jindal, explained that the corneal tissues were secured from eye banks in the US and brought to Guyana through the Subraj Foundation for the transplants to be done at the GPHC.
After screening approximately 60 candidates, Dr. Pasternak conducted the 16 corneal transplants between July 25-30 with assistance from the Head of the GPHC Ophthalmologist Department, Dr. Shailendra Sugrim and another local ophthalmologist, Dr. Celeste Hinds.
He explained that of the 16 corneal transplants conducted, two of the surgeries were conducted with the intention to save the eye; three to reduce pain with the understanding that vision may or may not be restored; and 11 were done with the intention to restore vision.
The results
Assessing the various cases, the Transplant Specialist disclosed that Grant was one of the two persons that will not be able to see following the surgery since the primary objective was to save the eye.
“He (Grant) may never be able to recover his vision because of the severity of the damage… The psychological impact of losing the eye is so dramatic, so we always try to save the eye even if there is no visual potential,” Dr. Pasternak explained.
“Three are doing it for pain control knowing that their visual potential is limited but the vast majority of the patients that we have selected, we selected them because they have the potential to see better,” he added.
Rajkumar, Kanhai and Britton were among those who underwent the surgeries with the intention of having their vision restored. Though patients were allowed to go home after their surgeries, it would take approximately one year before they fully recover.
Dr. Sugrim, in a separate interview, told the Pepperpot Magazine that on a daily basis the Eye Clinic sees between 200 and 300 patients. On a given day, he said there are usually about patients with cornea related issues.
According to him, every year, there are approximately 50 to 75 patients who would require a Corneal Transplant due to their corneas being damaged, however, only a limited amount of these patients have been able to undergo these surgeries. Today, GPHC has collaborated with the Subraj Foundation to carry out a total of 57 corneal transplants since 2015.
Plans for the future
To create greater access to the corneal tissues, the Subraj Foundation is analysing the possibility of setting up an Eye Bank here in Guyana to meet the needs of those patients desperately in need of Corneal Transplants.
Head of the Subraj Foundation, Tony Subraj, who took up the mantle upon the passing of his father George Subraj – the founder, said if an eye bank is established here in Guyana, the foundation in collaboration with GPHC would be able to carry out more transplants per year.
According to Subraj, he has already started to engage members of both sides of the National Assembly with the hope of effecting the necessary legislative changes to allow for an eye bank here.
Dr. Sugrim said that once the necessary legislative framework is put in place, the eye bank can be established within a period of two years.
He added that Dr. Hinds, who has recently returned to Guyana after completing a three months fellowship which focused on the cornea, has been mandated to lead the team that will assist with formulating the legislation.




.png)